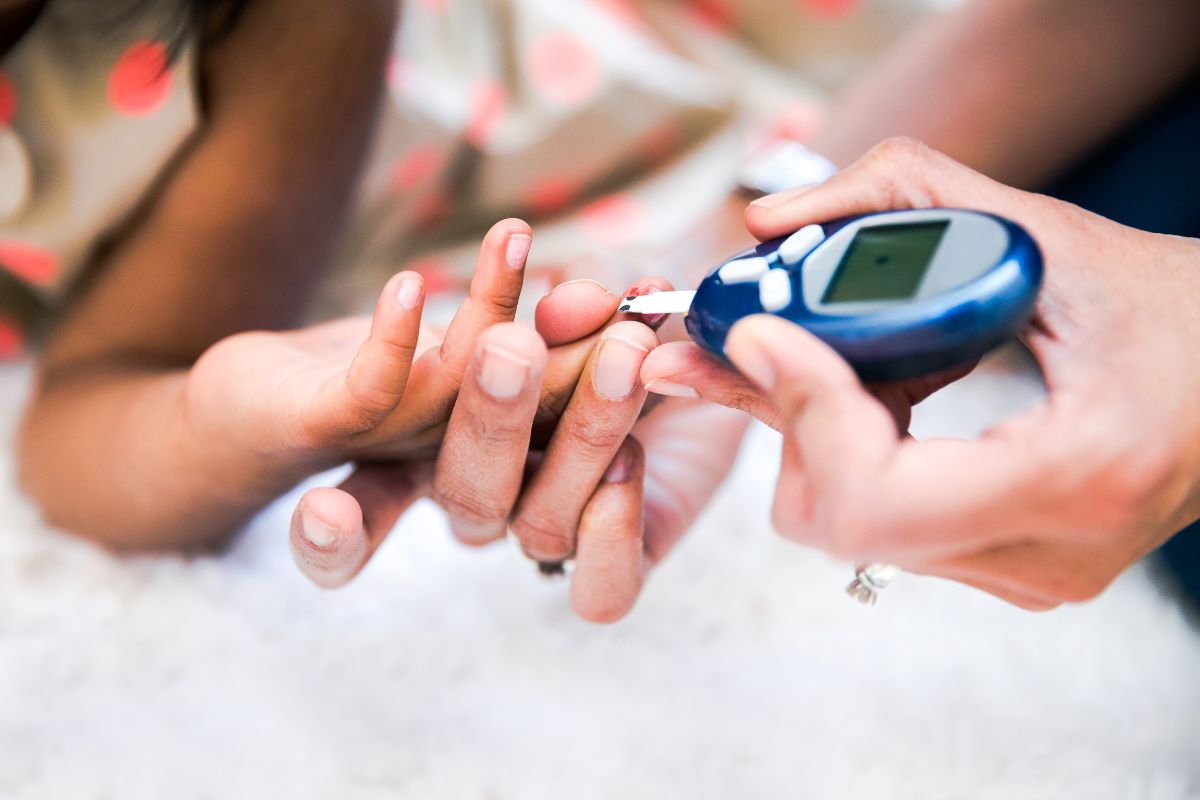
What is Type 2 Diabetes?
In this article we will discuss What is the Symptom of Type 2 Diabetes, Causes, Treatment and Prevention. Type 2 diabetes is a chronic condition that affects the way the body processes blood sugar (glucose).
It is characterized by insulin resistance, where the body’s cells do not respond effectively to insulin, and in some cases, the pancreas does not produce enough insulin. This leads to elevated levels of glucose in the blood, which can cause a range of health issues over time.

What is the Symptom of Type 2 Diabetes?
The symptoms of type 2 diabetes develop slowly and can include:
Increased Thirst and Urination
One of the hallmark symptoms of type 2 diabetes is increased thirst (polydipsia) and frequent urination (polyuria). This occurs because the kidneys have to work overtime to filter and absorb the excess sugar in your blood. When they can’t keep up, the excess sugar is excreted into your urine, dragging fluids from your tissues along with it.
This triggers more frequent urination, which can lead to dehydration and, as a result, increased thirst. People with this symptom may find themselves drinking and urinating more than usual, a cycle that can disrupt sleep and daily activities.
Increased Hunger
Increased hunger or polyphagia is another common symptom associated with type 2 diabetes. Despite eating more than usual, individuals may feel constantly hungry. This happens because the body’s cells are unable to get glucose from the blood (due to insulin resistance), leading the body to think it hasn’t been fed and to signal hunger. This can result in a vicious cycle of eating more, which in turn can exacerbate blood sugar levels and symptoms of diabetes.
Fatigue
Fatigue in people with type 2 diabetes can be profound and affect every aspect of their life. It arises from an inability of glucose to enter the cells efficiently due to insulin resistance. Without glucose, the body’s main source of energy, cells are starved for fuel, leading to feelings of tiredness and exhaustion. Additionally, high blood sugar levels can cause inflammation and increase oxidative stress, contributing further to fatigue.
Blurred Vision
Blurred vision is often one of the first warning signs of diabetes. High levels of glucose in the blood can lead to swelling of the lens in the eye, changing its shape and flexibility, and impairing its ability to focus, leading to blurred vision.
This symptom can fluctuate with blood sugar levels; as sugar levels normalize with treatment, vision often returns to its usual clarity. However, prolonged exposure to high blood sugar can cause permanent damage to the eyes, highlighting the importance of early detection and management.
Slow Healing of Cuts and Wounds
Individuals with type 2 diabetes may notice that cuts and wounds take longer to heal than expected. High blood sugar levels can impair blood circulation, leading to reduced oxygen and nutrient supply to the site of injury.
This can weaken the body’s defense mechanisms, slowing down the healing process and making it more susceptible to infections. Moreover, high sugar levels can impair the function of white blood cells, which play a crucial role in the healing process.
Tingling, Numbness, or Pain in the Hands or Feet
This symptom is a result of nerve damage (neuropathy) caused by prolonged high blood sugar levels. Over time, elevated glucose can damage the blood vessels that supply the body’s nerves, particularly in the extremities, leading to tingling, numbness, or pain in the hands and feet.
This can affect balance and coordination, making it difficult for individuals to perform daily tasks. Early diagnosis and management of diabetes can prevent or delay the progression of neuropathy.
Patches of Dark Skin
Patches of dark skin, particularly around the neck and armpits, may indicate a condition known as acanthosis nigricans, which is often associated with insulin resistance. These areas may feel velvety and may be a sign that your body is having trouble using insulin effectively, which is a common issue in type 2 diabetes.
The appearance of these patches can be a visible sign of the body’s struggle with insulin and may prompt individuals to seek medical advice, leading to the detection of diabetes or prediabetes.
What are the Causes of Type 2 Diabetes?
Type 2 diabetes is caused by a combination of genetic and lifestyle factors. Key contributors include:
Obesity or Being Overweight
Obesity is a primary risk factor for developing type 2 diabetes. Excess body fat, especially when distributed around the abdomen, can cause cells to become resistant to the effects of insulin. This insulin resistance forces the pancreas to produce more insulin to keep blood sugar levels under control.
Over time, this can lead to the pancreas becoming overworked and unable to produce enough insulin, causing blood sugar levels to rise. Maintaining a healthy weight through diet and exercise is a crucial step in preventing and managing type 2 diabetes.
Physical Inactivity
Physical inactivity is another significant risk factor for type 2 diabetes. Regular physical activity helps control weight, uses up glucose as energy, and makes cells more sensitive to insulin. Lack of exercise, therefore, contributes to weight gain and increases insulin resistance. Engaging in regular physical activity, such as walking, cycling, or swimming, can greatly reduce the risk of developing type 2 diabetes.
Poor Diet
A diet high in calories, processed foods, and unhealthy fats can contribute to the development of type 2 diabetes. Foods with a high glycemic index (which cause a rapid increase in blood sugar levels) can lead to insulin resistance over time. Conversely, a diet rich in fruits, vegetables, whole grains, and lean proteins can help maintain stable blood sugar levels and support a healthy weight, reducing the risk of diabetes.
Genetics and Family History
Type 2 diabetes has a strong genetic component. Individuals with a family history of diabetes are at a higher risk of developing the condition themselves. Genetics can influence an individual’s susceptibility to insulin resistance and can affect how the body stores fat, which are key factors in the development of diabetes. While genetic predisposition cannot be changed, lifestyle modifications can help mitigate the risk.
Age
The risk of developing type 2 diabetes increases with age. This is partly because people tend to exercise less, lose muscle mass, and gain weight as they age. Additionally, the body’s cells may become more resistant to insulin as a person gets older. However, type 2 diabetes is increasingly being diagnosed in younger populations, largely due to rising obesity rates.
High Blood Pressure and Cholesterol Levels
High blood pressure and abnormal cholesterol levels are common in people with type 2 diabetes and can contribute to the development of the condition. These factors can increase insulin resistance and are associated with the metabolic syndrome, which includes a cluster of conditions such as obesity, hypertension, and high blood sugar levels, further elevating the risk of diabetes.
Ethnicity
Certain ethnic groups, including African Americans, Hispanics, Native Americans, and Asian Americans, have a higher risk of developing type 2 diabetes. This increased risk is due to a combination of factors, including genetics, diet, lifestyle, and possibly socio-economic factors that affect access to healthy food and opportunities for physical activity. Understanding these disparities is crucial for targeting prevention efforts and improving health outcomes in these populations.
Diagnosis of Type 2 Diabetes
Diagnosis of type 2 diabetes is based on blood tests, including:
- Glycated hemoglobin (A1C) test, which measures average blood sugar level over the past 2 to 3 months.
- Fasting blood sugar test, taken after an overnight fast.
- Oral glucose tolerance test, measuring blood sugar after fasting and then again after drinking a sugary drink.

What is the Treatment of Type 2 Diabetes?
Type 2 diabetes, while not curable, can be effectively managed to minimize its impact on health and quality of life. Here’s a detailed look at the main treatment options:
Dietary Changes to Manage Blood Sugar Levels and to Lose Weight
Diet plays a crucial role in managing type 2 diabetes. A balanced diet that prioritizes whole, nutrient-dense foods over processed items can help control blood sugar levels and support weight loss efforts. Key dietary recommendations include focusing on vegetables, fruits, lean proteins, and whole grains while limiting saturated fats, refined carbohydrates, and sugars.
Portion control and meal planning can also help prevent spikes in blood sugar levels. For many, losing even a small amount of weight can significantly improve diabetes management and overall health.
Regular Physical Activity
Exercise is another cornerstone of type 2 diabetes management. Regular physical activity helps improve insulin sensitivity, which means your body can use the available insulin more efficiently to lower blood sugar levels. Additionally, exercise aids in weight management and can help reduce the risk of heart disease, a common complication of diabetes. Aim for at least 150 minutes of moderate-intensity aerobic activity per week, along with muscle-strengthening activities on two or more days per week.
Medications to Improve Insulin Sensitivity or to Stimulate the Pancreas to Produce More Insulin
There are various medications available to treat type 2 diabetes, each working in different ways. Some drugs increase insulin sensitivity, helping the body’s cells use insulin more effectively. Others stimulate the pancreas to produce more insulin.
Metformin, one of the most commonly prescribed medications for type 2 diabetes, works by reducing glucose production in the liver and improving insulin sensitivity. Depending on individual needs, other medications may be prescribed alone or in combination to achieve optimal blood sugar control.
Monitoring Blood Sugar Levels Regularly
Regular monitoring of blood sugar levels is vital for managing type 2 diabetes. It helps individuals understand how different foods, activities, and medications affect their blood sugar. It also provides critical information for making daily treatment decisions and adjustments.
Continuous glucose monitors (CGMs) and traditional blood glucose meters are tools that can aid in this ongoing process, helping to maintain blood sugar levels within the target range recommended by healthcare providers.
Insulin Therapy in Some Cases
While many people with type 2 diabetes can manage their condition with lifestyle changes and oral medications, some may require insulin therapy. This is more common in individuals who cannot maintain blood sugar control with other treatments or who have had diabetes for an extended period.
Insulin therapy involves injecting insulin to help control blood sugar levels, with the dosage and type of insulin tailored to each individual’s needs.
Effective management of type 2 diabetes requires a comprehensive approach that includes lifestyle modifications, medication as needed, and regular monitoring of blood sugar levels. Collaboration with a healthcare team, including doctors, dietitians, and diabetes educators, can provide the support and guidance needed to manage the condition effectively.

What is the Prevention of Type 2 Diabetes?
Preventing type 2 diabetes is largely about making positive lifestyle changes that address key risk factors. By adopting healthier habits, individuals can significantly lower their risk of developing this condition. Here’s a closer look at each preventive measure:
Maintaining a Healthy Weight
Excess body weight, especially when fat is mainly around the abdomen, increases the risk of developing type 2 diabetes. Fat cells in the abdomen are more than just storage; they can also have a direct impact on insulin resistance. Maintaining a healthy weight through balanced eating and regular exercise is crucial. Even a modest weight loss of 5% to 10% of total body weight can dramatically reduce diabetes risk.
Eating a Balanced Diet Rich in Fruits, Vegetables, and Whole Grains
A diet that emphasizes fruits, vegetables, and whole grains can help protect against diabetes. These foods are rich in fiber, vitamins, and minerals while being lower in calories and fat than many other types of food.
Fiber, in particular, can help control blood sugar levels. A balanced diet also limits intake of refined sugars and grains, which can cause blood sugar spikes and contribute to weight gain and insulin resistance.
Regular Physical Exercise
Regular exercise has multiple benefits for diabetes prevention. It helps control weight, lowers blood sugar levels, and improves insulin sensitivity. A mix of aerobic exercise (such as walking, swimming, or cycling) and resistance training (like weight lifting) is often recommended. Aim for at least 150 minutes of moderate to vigorous exercise each week, spread out over several days to ensure activity on most days.
Regularly Monitoring Blood Pressure and Cholesterol Levels
High blood pressure and high levels of cholesterol can exacerbate the risk factors for cardiovascular disease, which is also linked to an increased risk of type 2 diabetes. Regular monitoring, along with dietary changes and physical activity, can help keep these risk factors in check. In some cases, medication may be necessary to manage high blood pressure or high cholesterol.
Avoiding Tobacco Use
Smoking has a direct link to the development of type 2 diabetes. Nicotine can lead to insulin resistance, while the harmful chemicals in cigarettes can cause inflammation, both of which increase diabetes risk. Quitting smoking can improve overall health and significantly reduce the risk of developing type 2 diabetes, among other diseases.
By integrating these preventive measures into daily life, individuals can significantly reduce their risk of developing type 2 diabetes. It’s about creating a sustainable, healthy lifestyle, not just short-term changes. Regular check-ups with a healthcare provider can also help identify potential risk factors early and allow for prompt action to prevent diabetes.

Last word…
Early detection and management of prediabetes, a condition where blood sugar levels are higher than normal but not high enough for a diagnosis of diabetes, can also help prevent or delay the onset of type 2 diabetes.
It’s essential for individuals at risk of or diagnosed with type 2 diabetes to work closely with healthcare professionals to monitor and manage their condition effectively, preventing complications and maintaining a high quality of life.Wh